Scotoma
What is Scotoma?
A scotoma is an area in the human field of vision that is characterized by degeneration, hazy or even outright absence of sight surrounded by an area with normal vision. Eye sight can be impaired by a lesion anywhere on the visual pathway.
Complex and requiring a fine degree of diagnostic skill, multiple lesions from the occipital lobe of the brain all the way to the eyes may be responsible for the development of scotomas. Brain tumors, trauma, metabolic disorders or thromboembolic processes are on this inclusive list of cause of scotoma.
In order to understand the visual defects of scotoma, we will need to discuss about the anatomic and physiologic function of the visual pathway.
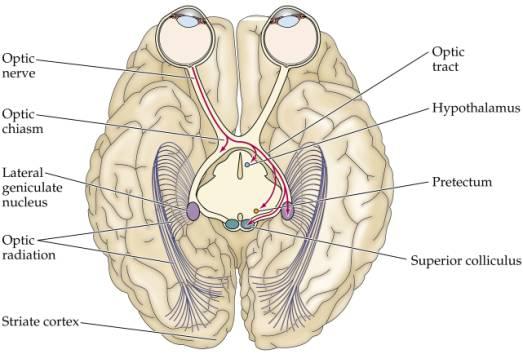
Image 1. The pathways of the visual system.
As you can see, this is a view of the brain from the bottom which shows the pathway of vision from the eyes to the optic nerves, optic chiasm and optic radiations going to the occipital lobe.
Pathogenesis of scotoma
The pathogenesis of scotoma need to be determined first where the lesion is, if the scotoma is limited to one eye, doctors can presume that the lesion is just before the optic chiasm as the optic fiber damage is limited to that particular eye.
This is very useful in determining the progression of glaucoma and pseudotumor cerebri. Scotomas are created in such a way that they match the anatomic area and the projection area affected. If the patient has a supra-nasal retinal detachment, the scotoma is an infra-temporal scotoma.
If the damage is to the macula, the scotoma is central. Glaucoma destroys the axons of the superior and inferior temporal poles of the optic disc resulting into an arcuate shaped scotoma that looks like a Turkish scimitar. Scotomas may also occur from optic neuritis, ischemic optic neuropathy, optic disc drusen and branch retinal artery or vein occlusion.

Image 2: An example of the visual field of a normal person versus one with a central scotoma.
About half of the optic fibers originate from the ganglion serving the macula. Damage here causes a central scotoma. If prolonged, the ischemic nature causes the disc to become pale and is noted to be irreversible. The presence of mass lesions in the sellar region causes a temporal hemianopia in each eye.
If the tumors are hemangiomas that are just in front of the optic chiasm, they will produce a combined scotoma that are characterized by optical neuropathy in one eye and superior-temporal cut in the other eye.
Asymmetric compression of the optic chiasm by a pituitary adenoma, meningioma, craniopharyngioma or aneurysm results into bitemporal hemianopia. Insidious development of this condition causes it to be detected only when the physician examines each eye separately.
It is difficult to localize a post-chiasmal lesion as this could be anywhere along the optic tract, geniculate body, optic radiations and the occipital lobe. A unilateral post-chiasmal lesion will leave the visual acuity in the eye unaffected. Lesions in the optic radiations will result into poorly localized and incongruent eye defects in both eyes.
Damage to optic radiations in the temporal lobe (Meyer’ Loop) will result into superior quadrantic homonymous hemianopia. Injuries to optic radiations in the parietal lobe will result into inferior quadrantic homonymous hemianopia.
Lesions in the occipital lobe will result into a mixed dense congruous eye defects in both eyes. Ischemia is also implicated in development of total homonymous hemianopia, occlusion of the posterior cerebral artery results into this defect.
Destruction of the occipital lobe results into total blindness; this is different from prechiasmal loss by the presence of intact pupillary responses.
Treatment of Scotoma
Given the variety of lesions that occur in the visual tract pathway, it’s the business of physician to determine the exact location of the lesion or in the absence of such physical lesions, medical conditions that could be the cause of such disruption in the visual fields.
It is imperative that the patient seek immediate medical attention as treatment in the early hours of detection of the visual field effect preserves vision. If the patient delays or the condition is inherently irreversible, these scotomas may persist. This is why we need to have excellent education drives to improve the awareness of people of the devastating effects of scotoma.
Underlying causes of scotoma should be determined as early as possible. In the cases of tumors that affect anywhere along the visual tracts, a good history and physical examination of the eyes plus a good radiologic examination in the form of CT scans or MRI can help localize the lesions.
Once identified, treatment will include precise, surgical excision of the tumor. The prompt excision of these tumors will help correct the scotomas by relieving the pressure effects of the mass on the sensitive visual tract pathway. If the cause is more of cardiovascular in nature, management of hypertension will be needed to prevent ischemia of the small caliber arteries of the eye which may result into the visual loss.
If the scotoma is not treated early, the damage will indefinitely persist and as of the moment, no medical therapies exist for correcting the visual field defects.
Conclusion
Indeed scotomas are devastating. They are a result of any lesions that affects the visual tract pathway. These lesions may the result of direct trauma, benign or malignant neoplasms with mass effects and cardiovascular like hypertension. People need to be informed about these devastating effects so that prompt treatment can be initiated to preserve eye sight.
